What is DOH Clinical Costing?
Clinical costing is the process of measuring the actual cost of delivering patient care by tracking resource usage at a detailed level.
Instead of looking at costs broadly, it focuses on:
-
Individual patient encounters
-
Specific services and procedures
-
Actual resource consumption
This allows healthcare providers to understand the true cost of care delivery.
To put it simply:
-
Billing shows what you charge
-
Clinical costing shows what it actually costs you
This difference is critical. Without it, providers often operate without real financial clarity.
To better understand this foundation, it’s important to explore how patient-level costing in healthcare works, since it forms the backbone of the entire DOH framework.
Why Clinical Costing is Mandatory in Abu Dhabi
The shift toward clinical costing is part of a broader transformation in the healthcare system.
The Department of Health – Abu Dhabi is moving toward a value-based healthcare model, where providers are evaluated not just on volume, but on efficiency, outcomes, and cost transparency.
To support this, a centralized system has been introduced for cost data collection and benchmarking across providers.
This means your data is no longer just internal — it is used for comparison, analysis, and decision-making at a system-wide level.
If you’re unsure whether your facility is aligned with current expectations, reviewing a DOH compliance checklist for healthcare providers can help identify gaps early.
Clinical Costing 2026 Submission Timeline
For 2026, the official submission cycle is clearly defined:
- Preparation Phase: Must be completed before August
- Data Submission Window: August 1st to August 31st
- Validation & Review: Conducted after submission.
Who Needs to Comply?
Clinical costing applies to all licensed healthcare providers in Abu Dhabi, including:
-
Hospitals
-
Day surgery centers
-
Rehabilitation facilities
-
Specialized services such as dialysis, IVF, and dental care
-
Clinics and primary care centers
In short, if your facility is licensed, compliance is mandatory regardless of size.
Core Components of DOH Clinical Costing
Clinical costing is not a single process — it is a structured system made up of multiple components that must work together.
1. Cost Center Structure
Healthcare providers must define cost centers based on their operational structure. These are typically divided into:
-
Direct cost centers (patient care related)
-
Overhead cost centers (support functions such as HR, IT, finance)
These cost centers must also be mapped into standardized reporting groups, ensuring consistency across all providers.
2. Cost Types
All expenses must be categorized into standardized cost types such as:
-
Staff salaries (clinical and non-clinical)
-
Laboratory and imaging
-
Pharmacy and consumables
-
Medical supplies
-
Overheads and depreciation
This ensures that financial data is structured uniformly across facilities.
3. Patient-Level Costing
At the core of the DOH framework is patient-level costing.
Healthcare providers must link costs directly to:
-
Patient encounters
-
Services delivered
-
Resource usage
This level of detail requires a strong costing model, and many providers rely on activity-based costing in healthcare to achieve accurate results.
4. Data Requirements
Clinical costing depends heavily on data integration.
Providers must combine data from:
-
Financial systems (general ledger)
-
Clinical systems
-
HR and payroll
-
Inventory and supply systems
If your data is fragmented, your costing accuracy will be affected.
5. Cost Allocation Methodology
Cost allocation is one of the most technical parts of the process.
Overhead costs must be distributed using logical methods such as:
-
Reciprocal allocation
-
Step-down allocation
More importantly, allocation must reflect actual resource usage.
If you’re unfamiliar with how this works, understanding cost allocation in healthcare systems is essential before implementation.
6. Cost Buckets and Standardization
To ensure consistency, services are grouped into standardized categories such as ICU, imaging, laboratory, pharmacy, and ward services.
This allows benchmarking and comparison across healthcare providers.
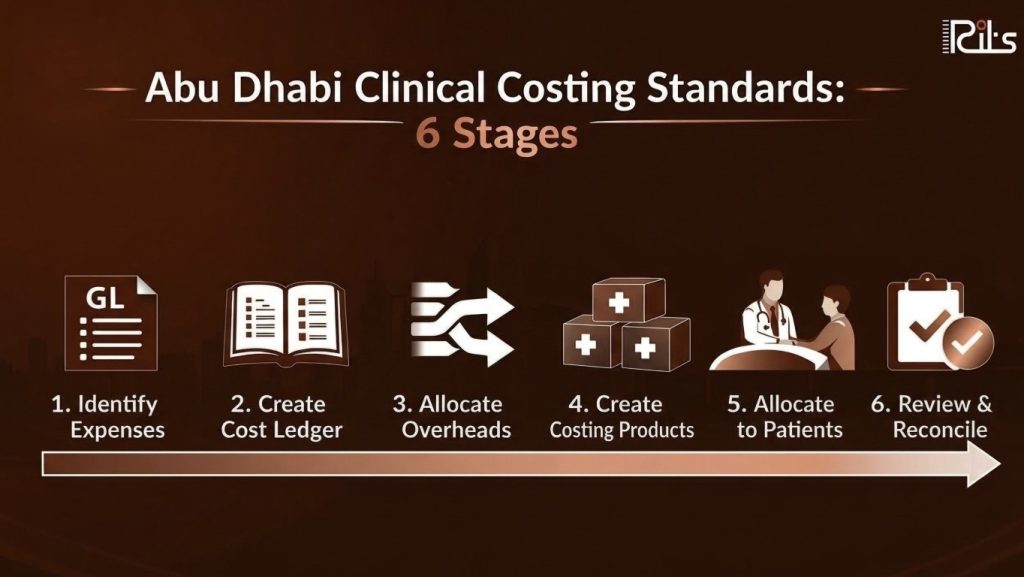
DOH Clinical Costing Process (Step-by-Step)
Clinical costing follows a structured workflow.
-
Collect all financial and operational data
-
Map costs to cost centers
-
Allocate overheads using approved methods
-
Define costing products (services and activities)
-
Assign costs to patient-level data
-
Validate and reconcile all data before submission
Each stage must be completed accurately to avoid errors during submission.
If you want a deeper breakdown of how this works in practice, you can refer to a clinical costing submission process guide, which outlines each step in detail.
Common Challenges Healthcare Providers Face
Despite clear guidelines, many providers face challenges such as:
-
Disconnected systems
-
Incomplete or inconsistent data
-
Lack of internal expertise
-
Complex allocation logic
Another major issue is documentation.
Healthcare providers are expected to maintain detailed records of:
-
Costing methodologies
-
Allocation decisions
-
Data sources
If not handled properly, these issues often lead to errors. Many of these gaps can be identified early by reviewing a clinical costing compliance checklist, which helps highlight weaknesses in data, processes, and documentation before they impact submissions.
Risks of Non-Compliance
Failing to comply with clinical costing requirements can lead to serious consequences.
These include:
-
Regulatory penalties
-
Submission rejections
-
Increased audits
-
Operational disruptions
With the upcoming clinical costing deadline in Abu Dhabi for 2026, delaying implementation can increase compliance risks significantly.
Benefits of Clinical Costing (Beyond Compliance)
While compliance is the primary driver, clinical costing offers long-term benefits.
It helps healthcare providers:
-
Understand true cost drivers
-
Improve operational efficiency
-
Optimize resource allocation
-
Make better financial decisions
When implemented properly, it becomes a strategic tool rather than just a regulatory requirement.
How to Get DOH Clinical Costing Ready
A structured approach is essential for successful implementation.
Healthcare providers should:
-
Assess current systems and data readiness
-
Align financial and clinical data
-
Define cost centers and cost types
-
Implement allocation methodologies
-
Validate and reconcile data before submission
As the process becomes more complex, especially during allocation and data reconciliation, many providers transition toward using a clinical costing software to reduce manual effort and improve accuracy.
With the right system in place, along with a clearly defined process, healthcare providers can move toward full compliance with greater confidence and fewer errors.
Choosing the Right Clinical Costing Solution
By this stage, most healthcare providers realize that clinical costing is not just a finance task — it involves systems, structured data, and strict compliance requirements.
One of the first steps is understanding whether your current setup can support DOH standards. If you’re unsure, reviewing a clinical costing compliance checklist can help identify gaps before moving forward.
Once the gaps are clear, execution becomes the next challenge.
Manual processes and disconnected systems often lead to inaccurate allocations and delays. This is where having a dedicated clinical costing software becomes essential, as it helps streamline data integration, automate allocation logic, and ensure consistency in reporting.
QC Centra is designed by RITS and is one of the best clinical costing software in UAE providing a structured system aligned with DOH requirements. Backed by the expertise of RITS, it supports healthcare providers in building accurate, audit-ready clinical costing models.

Final Thoughts
The Abu Dhabi Clinical Costing Standard is a comprehensive framework that changes how healthcare providers manage and report costs.
It requires:
-
Structured data
-
Accurate methodologies
-
Continuous validation
And most importantly, it requires preparation.
Delaying implementation or treating it as a one-time task can lead to long-term issues.
The key is to start early, build the system correctly, and ensure your facility is fully aligned with DOH expectations.












